When it comes to rapid industry growth, few sectors are experiencing the explosive boom of the healthcare market. Shifting population demographics mean more and more adults are aging into the 65+ bracket and that translates into rising healthcare needs, including a growing demand for nurses and other healthcare workers.
The U.S. Bureau of Labor Statistics projects that healthcare support occupations are going to increase almost 25 percent over the next decade, faster than any other occupational vertical. As more and more people turn to nursing and healthcare support positions for a career, it’s important to understand what injuries are involved with one of the most hazardous industries out there. Don’t miss this essential guide to the top nursing injuries (with tips for preventing them too):
Back Injuries
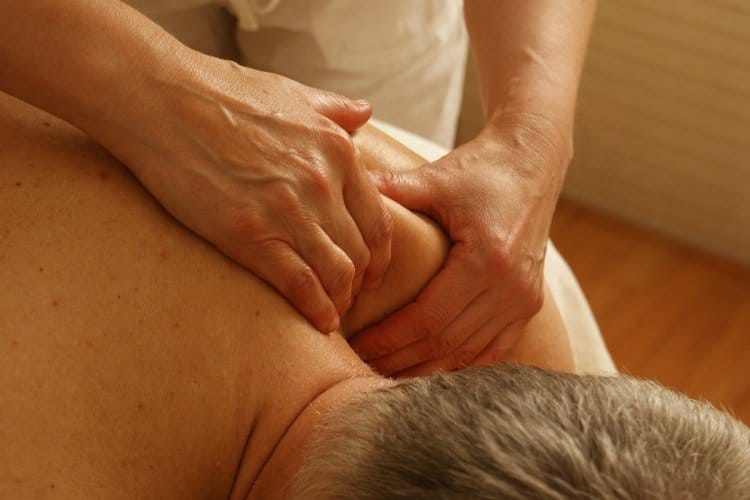
The incidence rate of musculoskeletal disorders among nurses is higher than any other occupation including truck drivers, warehouse workers, and baggage handlers. What factors contribute to this disturbing statistic?
Well not only do nurses have to manually handle patients to reposition, lift, transfer, and assist them with standing and sitting, but rising rates of obesity and longer average life expectancies have them doing it with heavier and heavier patients, many of whom are older and require extra support.
Certified nursing assistants and nursing aides also tackle physically-demanding tasks like bathing patients, changing bed sheets with patients in them, and tending to more immobile elderly patients in nursing homes.Common back injuries among nurses and nursing assistants include:
-
Chronic back and/or neck pain
-
Herniated disk (acute disk disease)
-
Low back strain
-
Sciatica (sciatic nerve pain in the back and legs)
So are all nurses doomed to some sort of back injury in their career? Not necessarily. New health and safety standards across hospitals and other healthcare institutions nationwide are requiring administrators to provide more tools and resources to prevent musculoskeletal injuries. For example, nursing staffs should always have access to lift devices (like Hoyer lifts, lift belts, and transfer chairs) and there should be an established protocol for calling back-up in the event that a patient falls and needs help getting up.
Nurses can also practice good spinal care by learning correct lifting techniques, wearing proper-fitting footwear during long shifts, and exercising regularly to strengthen core and back muscles.
Assault

Unfortunately, patient physical and verbal assault is not a foreign experience to nurses. In fact, 1 in 4 nurses surveyed says they have been assaulted at least once on the job. So how does violence against nurses happen in the first place?
As resources to address opioid addiction, untreated mental illness, and substance abuse in the community continue to fall short, rates of violence, especially in hospital settings continues to climb. Nurses may experience patients yelling at them, biting, scratching, or hitting them, and sometimes even worse assault. Not only is this occurrence frightening and stressful for a nurse, but it ends up eliminating a crew member from the staff for the shift as the nurse herself has to go get treated for injuries. This only heavies the burden nurses bear and fosters an ever more stressful work environment.
Hospital workers continue to work with the Occupational Safety and Health Administration on protocols and resources that can prevent violence against staff. Some avenues include working more closely with local police, training nursing staff in de-escalation tactics, practicing awareness drills, and establishing better nationwide standards for nurse protection.
Varicose Veins

Many jobs in the healthcare setting involve standing for prolonged periods of time, but it is nurses especially who tend to spend long shifts working on their feet. The nature of the job, therefore, increases a nurse’s risk for developing varicose veins.
There are tiny valves in the blood vessels in the feet and legs which are responsible for supporting the transport of blood against the force of gravity back up towards the heart. When these micro-ducts become dysfunctional due in part to frequent and prolonged standing or sitting, they allow blood to pool, creating dark, enlarged and bulging veins which may be accompanied by pain, fatigue, and tenderness. Varicose veins can also make a nurse more vulnerable to clotting incidents like you see with deep vein thrombosis.
To avoid developing varicose (and spider) veins, nurses should alternate sitting and standing as much as possible on the job. Wearing compression socks for nurses and elevating your feet at the end of the day to help usher blood upwards through the legs are also key ways to keep blood from pooling.
Illness
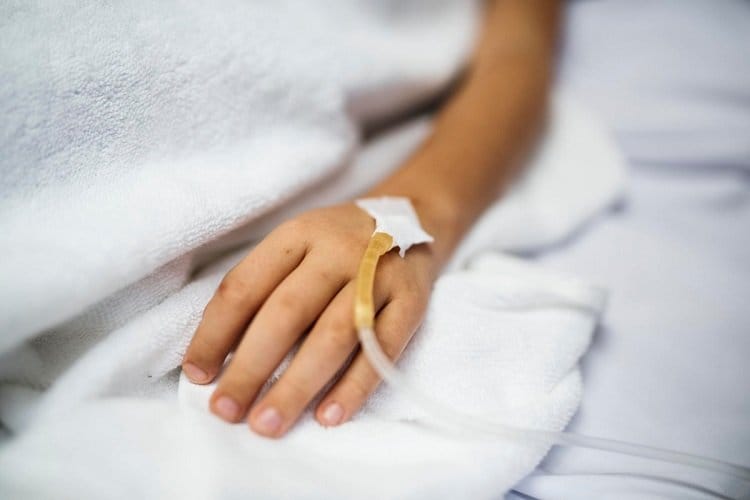
Frequent contact with patients who have highly-contractible infections like the influenza virus makes nurses and nursing assistants more susceptible to falling ill. Constant stress and sleep deprivation which often accompany a 12-hour shift (especially double shifts) can also have negative impacts on a nurse’s health.
In addition to age-old practices like washing hands frequently, being cautious about shaking hands with patients and their families, and consistently cleaning surfaces patients have touched, nurses can take added steps to safeguard their immune system. Exercising regularly and eating a healthy diet of whole foods (fruits, vegetables, whole grains, lean proteins, legumes, nuts, and seeds) can fortify the body against foreign pathogens and keep gut bacteria in balance.
Spending time outdoors and seeking stress-relief practices like yoga or meditation also plays an important role in a nurse’s overall wellbeing.

